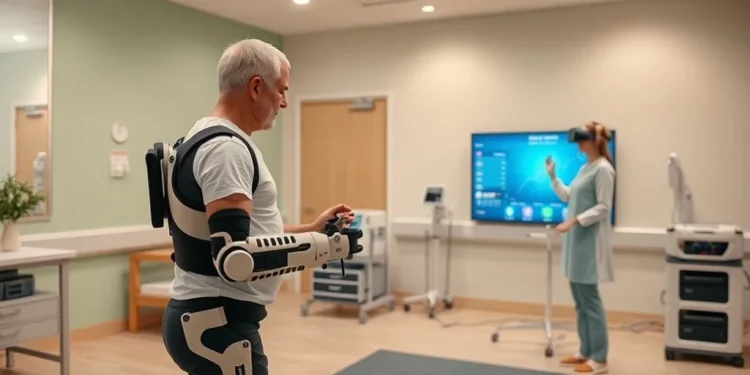
Imagine the terrifying, chaotic aftermath of a severe stroke. A 78-year-old patient survives the initial neurological trauma and is stabilized in the intensive care unit. The attending physician, reviewing the patient’s lingering mobility issues, prescribes a 20-day stay at an inpatient skilled nursing facility (SNF) for intensive physical and occupational therapy. This is the standard, medically necessary protocol for helping a survivor relearn how to walk, swallow, and regain their independence.
However, less than a week into the rehabilitation, the family receives a sudden, devastating notice from their insurance provider: coverage for the facility is being terminated. The patient must be discharged home immediately, or the family will have to pay thousands of dollars out-of-pocket per day.
The attending doctor is baffled; the patient is clearly not ready to go home. So, who overruled the physician?
Increasingly, the answer is not a medical director or a human claims adjuster. The decision to cut off care was made by an algorithm.
The integration of Artificial Intelligence (AI) into modern healthcare administration is rapidly changing the landscape of how care is approved, denied, and managed. While AI has the power to streamline administrative bloat, its aggressive use in determining the length of post-acute care is sparking outrage among patient advocates, families, and healthcare providers.
The Rise of Algorithmic Medicine
To understand how an algorithm gets to decide a patient’s medical fate, we have to look at how modern retirement healthcare is structured.
Over the last decade, there has been a massive shift away from Original Medicare where the government pays doctors directly for the services they provide toward Medicare Advantage (MA). Medicare Advantage plans are run by private, for-profit insurance companies that are paid a set fee by the government to manage a senior’s care.
Because these private companies keep whatever money they do not spend on patient care, they are heavily incentivized to control costs. One of the most expensive phases of medical care is the post-acute recovery period in a skilled nursing facility.
To tightly manage these costs, major insurers have quietly contracted with third-party tech companies that utilize predictive algorithms and machine learning models.
How the AI Calculates “Recovery”
These proprietary algorithms are fed massive datasets containing the medical histories of millions of past patients. When a new patient is admitted to a rehab facility following a stroke, a fall, or a joint replacement, their basic demographic and medical data (age, primary diagnosis, comorbidities) is plugged into the system.
The AI then compares the patient to its database and predicts exactly how long their recovery should take. For example, the algorithm might determine that the “average” 78-year-old female who suffered a mild ischemic stroke requires precisely 12.4 days of inpatient rehabilitation before she can be safely discharged.
On day 12, the system automatically flags the patient’s file for discharge. If the facility requests more time because the patient is still struggling to stand unassisted, the algorithm often generates an automatic denial.
The Human Cost of the “Average” Patient
The fundamental flaw in this system is that human beings especially seniors with complex, compounding health issues do not heal on a mathematically average curve.
A predictive model might calculate recovery based on a stroke, but it fails to properly account for the fact that the patient also has mild dementia, severe arthritis, and lives in a two-story home with no ramp. The AI operates in a frictionless, digitized reality, while the patient is recovering in a fragile, physical body.
When an algorithm cuts off care prematurely, the results can be catastrophic. Families are suddenly forced to become full-time medical caregivers overnight, without the necessary training or equipment. Often, patients who are discharged too early deteriorate quickly at home, resulting in a readmission to the emergency room just days later a cycle that is both physically traumatic for the patient and ultimately more expensive for the healthcare system.
The Regulatory Pushback
The rapid deployment of these predictive models has not gone unnoticed. Investigative journalists, Senate committees, and patient advocacy groups have recently highlighted the alarming rate of algorithm-driven care denials.
In response, the Centers for Medicare & Medicaid Services (CMS) issued a stark clarification to private insurers. The new guidelines strictly state that an algorithm or software tool cannot be the sole basis for denying care or overriding a human doctor’s clinical judgment. Insurers must ensure that medical necessity determinations are based on the individual patient’s specific circumstances, not just a broad, predictive data set.
However, enforcement remains a complex challenge. Insurers argue that these tools are merely “decision support” aids to help human medical directors manage the vast volume of claims, but doctors on the front lines report that overturning an algorithmic denial is an exhausting, bureaucratic nightmare of endless phone calls and appeals.
Navigating the New Reality
For families, the era of algorithmic medicine means that being a passive recipient of healthcare is no longer an option. Advocacy is now a mandatory part of the recovery process.
Navigating the complexities of senior insurance services now requires not just understanding premiums and copays, but understanding the mechanics of how claims are processed and denied. If a loved one is suddenly issued a discharge notice from a rehab facility that contradicts the attending doctor’s advice, families must immediately file an expedited appeal. In many cases, simply initiating the formal appeals process forces the insurer to put a human medical director on the case, which frequently results in the algorithmic denial being overturned.
Conclusion
The promise of artificial intelligence in healthcare is vast it has the potential to catch missed diagnoses, accelerate drug discovery, and eliminate billing fraud. But when it is used as a blunt instrument to aggressively restrict post-hospital care, it strips the humanity out of the healing process. Healing takes time, patience, and individualized care three things that a cost-saving algorithm is fundamentally programmed to ignore.